5 minutes
1077 words
How to Interpret Your Sleep Apnea Test Results
Catharine Nixon
September 12, 2022
Undergoing a sleep apnea test is a very important step in finding the proper treatment for sleep apnea disorder. It can be the difference between a normal, healthy life and one that is plagued by fatigue, daytime sleepiness, and other serious health problems. There are a few different types of sleep apnea tests that can be performed in order to diagnose the condition.
A sleep study is an assessment used to build a differential diagnosis of sleep disorders, including sleep apnea. It consists of applying electrodes to the scalp or midback, monitoring either your brain waves, blood oxygenation, heart rate, breathing while you sleep, or all of the above. A sleep study may be performed in a specialized sleep center or at home, using a portable test kit.
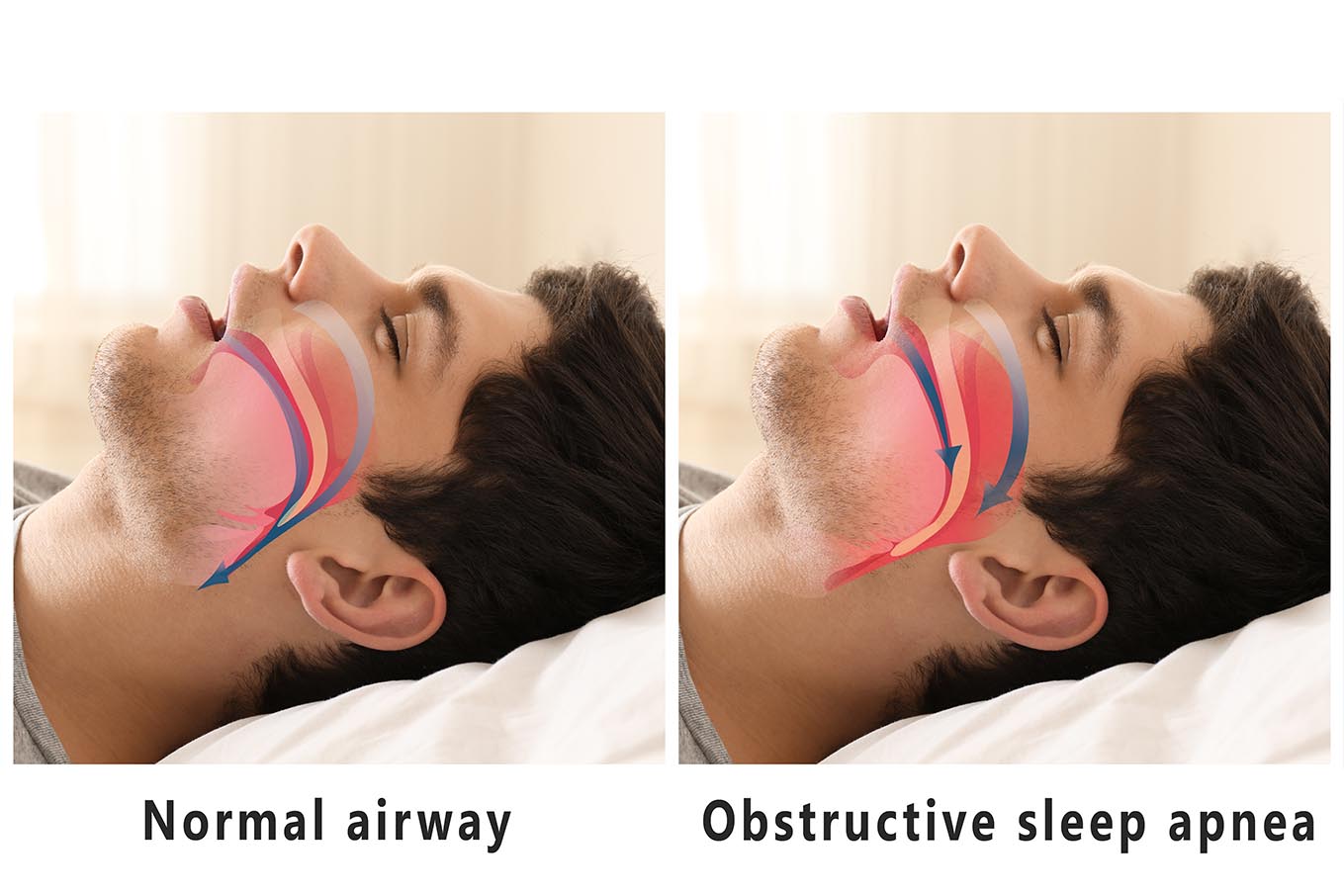
Types of Sleep Apnea Tests
There are a number of tests used to identify sleep apnea, but there are three main types of sleep apnea tests that are commonly used in diagnosis: the Polysomnogram, the Oximetry test, and the home sleep test.
The Polysomnogram is the most common type of sleep apnea test. This test is usually conducted at a sleep center. During the polysomnogram, sensors are placed on your body to measure your heart rate, blood oxygen level, brain waves, and breathing during sleep.
The Oximetry test measures the oxygen level in your blood. A sensor is placed on your finger or earlobe to measure your oxygen level while you sleep. Sleep apnea disrupts breathing and so blood oxygenation levels are supressed during sleep.
The home sleep test is the easiest way to monitor your breathing while you sleep. A small device (called a pulse oximeter) is placed on the finger or earlobe and records your oxygen level during the night. The device is attached to a computer and then analyzed by a doctor. This test can be done in the comfort of your own home and usually takes less than one hour.
Apnea-Hypopnea Index (AHI)
Apnea-Hypopnea Index (AHI) – what is it and how does it determine sleep apnea severity?
An Apnea-Hypopnea Index (AHI) is a number used to describe the severity of sleep apnea. It is calculated by dividing the total number of apneas and hypopneas by the total hours of sleep.
AHI results can range from 0 to over 100. The higher the number, the more severe the sleep apnea. AHI results are used to diagnose sleep apnea and determine how it should be treated. The AHI measures the number of apneas and hypopneas per hour of sleep. The severity of sleep apnea is determined by how often breathing stops or becomes very shallow during sleep and also by how much oxygen levels in the blood drop during these episodes. It is considered normal if the AHI is less than 5 per hour. If the AHI is greater than 30, it is considered severe sleep apnea.
The mean oxygen saturation (SaO) is a measure of how much oxygen is in the blood. It is calculated by dividing the average oxygen saturation over the night by 100. Patients with a SaO of less than 90% are considered to have severe sleep apnea.
Possible Sleep Apnea Test Results and What This Means for You
There are four possible results from a sleep apnea test: normal, mild, moderate, or severe.
Negative Sleep Study or Normal
A normal result on a sleep apnea test is an AHI of 5 or less. This means that the person has fewer than 5 apneas per hour and that each apnea lasts for less than 10 seconds. People with an AHI of 5 or less generally do not have symptoms of sleep apnea and do not need treatment.
If your sleep apnea test results come back as normal, that means you don’t have sleep apnea and you can stop worrying about it. However, if you’ve been experiencing symptoms of sleep apnea, such as loud snoring or feeling exhausted during the day, it’s worth seeing a doctor to rule out other possible causes.
Mild Sleep Apnea
Mild sleep apnea is diagnosed when the AHI, or apnea-hypopnea index, is between 5 and 15 events per hour. This means that mild sleep apnea sufferers experience 5 to 15 periods of time when they stop breathing or have shallow breaths per hour. The good news is that mild sleep apnea is often treatable with lifestyle changes, such as losing weight, sleeping on your side, and avoiding alcohol before bedtime.
Moderate Sleep Apnea
Patients with moderate sleep apnea results may have an AHI of 15 to 30. This means that they have 15 to 30 episodes of apnea per hour. While this is not as severe as those with severe sleep apnea, it can still lead to serious health consequences.
Your doctor can help you find the right treatment options for your needs. Treatments for mild and moderate sleep apnea are very similar such as lifestyle changes, losing weight, and quitting smoking. In some cases, you may also need to use a continuous positive airway pressure (CPAP) machine to help you breathe at night.
A different treatment option is a surgery called upper airway surgery. This helps widen the airway so that breathing can be normalised during sleep. This is usually a last resort however, as this surgery is quite intensive.

Severe Sleep Apnea
Severe sleep apnea is a serious medical condition that can have potentially life-threatening consequences. It is characterized by a high number of apneic episodes per hour of sleep. Sleep apnea is considered severe if the AHI is greater than 30. People with severe sleep apnea are at increased risk for high blood pressure, heart disease, stroke, and other health problems.
However, additional testing is often required to determine the level of severity and to narrow down available treatment options. When OSA is classified as being severe, other reasons of severity need to be considered, including the presence of central sleep apnea, and Cheyne-Stokes breathing pattern, which signifies advanced disease and which calls into question the feasibility and safety of all treatment options.
In conclusion, untreated sleep apnea can have serious consequences. It can lead to high blood pressure, heart disease, and stroke. It can also cause problems with memory and concentration, and increase the risk of accidents. If you think you may have sleep apnea, it’s best to talk to your doctor.

